Abstract: The biopsychosocial-nutritional model of medicine proposes a holistic approach to health, viewing the body as a complex adaptive system that is influenced by biological, psychological, social, and nutritional factors. This model aligns with the evolutionary-stress framework, emphasizing the role of stress and energy dynamics in health and disease. This article introduces the biopsychosocial-nutritional model and discusses its place within the evolutionary-stress framework.
Introduction
Modern medicine traditionally operates from a biomedical model that focuses largely on biological factors in health and disease. However, an emerging perspective, known as the biopsychosocial-nutritional model, views health and disease through a more holistic lens. This approach recognizes the human body as a complex adaptive system, acknowledging the interplay of biological, psychological, social, and nutritional factors in health outcomes.
The Biopsychosocial-Nutritional Model of Medicine
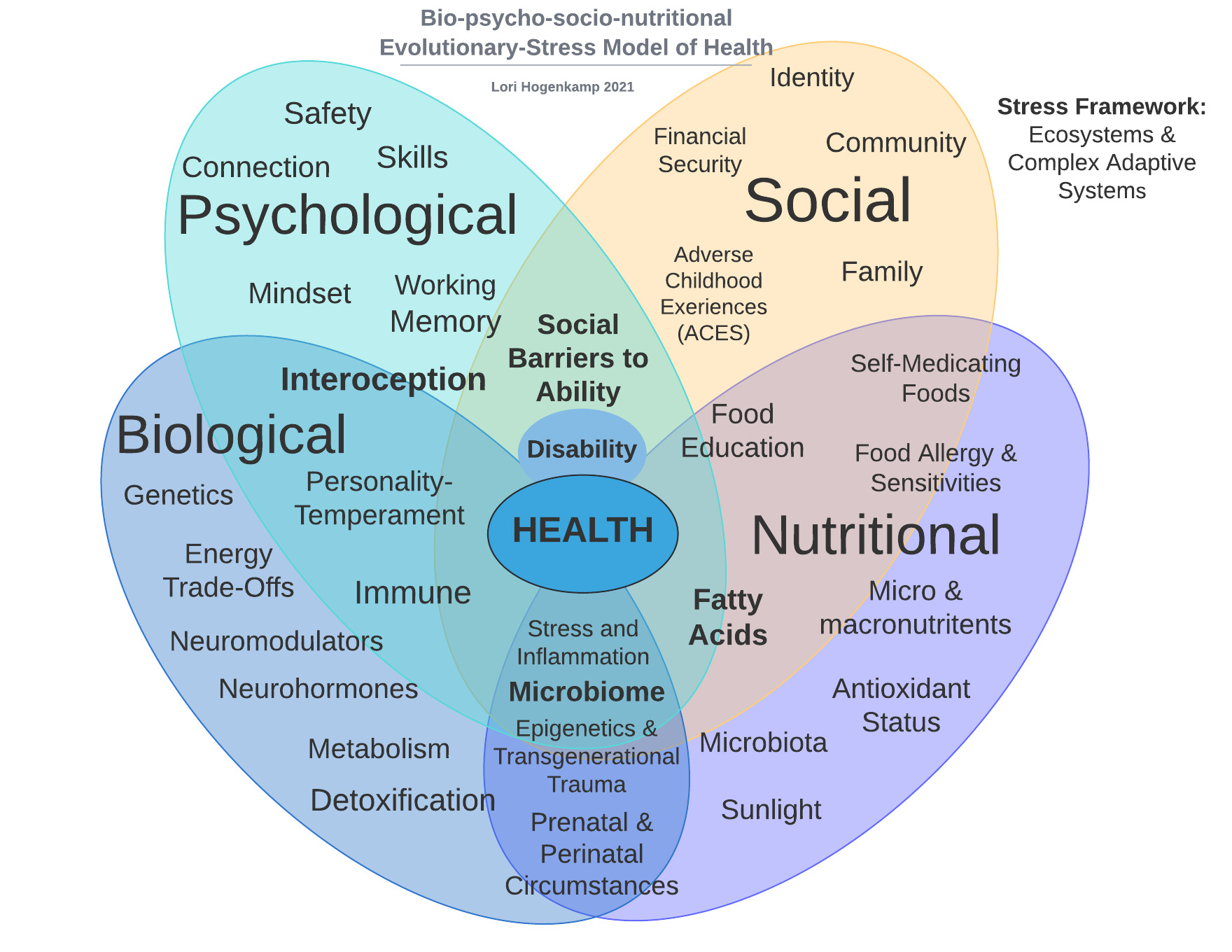
The biopsychosocial-nutritional model is a comprehensive approach to health and disease. It posits that biological processes, psychological states, social conditions, and nutritional factors interact in complex ways to influence health outcomes.
Biological factors encompass elements such as genetics, physiology, and neurobiology. Psychological factors consider mental states, behaviors, and emotional health. Social factors encompass social relationships, cultural contexts, and socioeconomic status. Nutritional factors, a key component often overlooked, involve dietary patterns, nutrient intake, and metabolic health.
The model asserts that these different areas interact dynamically within an individual, making health a product of multifaceted interplay. This understanding emphasizes the importance of personalized, holistic health care that considers the whole person and their environment.
The Evolutionary-Stress Framework and the Biopsychosocial-Nutritional Model
Stress is seen as a fundamental communication network within the body, and the mediary between our genes and the environment. The body’s energy dynamics play significant roles in the complex adaptive system of the human body.
Stress and energy dynamics, under the evolutionary-stress framework, form part of the biological sphere but interact strongly with the psychological, social, and nutritional aspects of health. Stressors can arise from any of these areas, and the body’s response to stress can influence all of them. Nutrition, in particular, plays a dual role, both as a source of potential stressors (such as dietary deficiencies or excesses) and as a vital resource for managing stress and maintaining energy balance.
The Neuromatrix
NeuroMatrix is a term coined to encapsulate the intricate interplay and bidirectional communication occurring among the brain, immune system, endocrine system, and gut microbiota. The concept embodies an interconnected network where each component does not function in isolation but rather influences and is influenced by the others. These interactions contribute to cognitive-learning styles, stress responsivity, personality and temperament variation, and have implications for the understanding of health and disease.
The NeuroMatrix concept appreciates the robust and dynamic connections that exist within this network, emphasizing that these systems work in a coordinated fashion to regulate various physiological and psychological functions. It is through the NeuroMatrix that one can understand the trade-offs that result from the inherent diversity of human neurobiology and how this impacts health outcomes.
Conclusion
The biopsychosocial-nutritional model offers a holistic perspective on health and disease that aligns with the evolutionary-stress framework’s focus on stress and energy dynamics. It emphasizes the complex interactions of biological, psychological, social, and nutritional factors in health outcomes, highlighting the importance of personalized, holistic approaches to health care. As our understanding of these interactions deepens, the potential to improve health outcomes through more comprehensive, person-centered care approaches becomes increasingly evident.